Bowel movements are one of the best gauges of health. So it’s unfortunate to hear that people are uneducated on the topic, and ignoring clear signs of dysfunction.
But perhaps we can blame western medicine for that – as they’d rather take your blood pressure, look in your ears and write-up a prescription then ask about your diet and lifestyle…or the last time you pooped!

Realistically, the quality (shape, size, color, odor, sound) and schedule of your bowel movements can give you a red flag that’s something is wrong before it actually is (and long before you have to go to your doctor). And if you start paying more attention to it on a “regular” basis, you can adjust accordingly; whether that’s drinking more water, avoiding specific foods, increasing specific foods, or simply taking a stress break.
Unfortunately, there’s no one-size-fits-all with schedule – as some people simply poop more than others – but there is a one size fits all with quality. Which extends far beyond the giant floaters the Fiber Frauds have you shooting for.
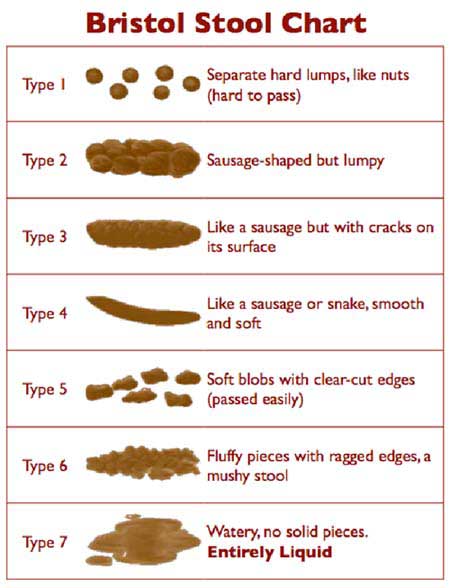
As depicted in the chart above (from here), the perfect poop is a Type 4 with all of the characteristics below:
- medium to light brown and all 1 color
- smooth, soft and in one piece
- 1-2 inches thick and a long S-shape
- enters water like an Olympic diver (quiet, no splash)
- smell is manageable
- floats at first and sinks slowly
Despite conventional thinking, The Perfect Poop is not achieved with MORE fiber, and MORE whole grains. Since the harder stools (types 1-3) that are hard to pass are not a ‘volume’ problem, they’re an ‘evacuation’ problem. And other than the gut inflammation that comes with trying to add indigestible roughage, this illadvised strategy simply adds ‘more poop’ – which does NOTHING for constipation and only stretches and damages the GI tract.
For instance, a study from 2012 in the World Journal of Gastroenterology moved 63 middle-aged individuals with constipation (going less than every 3rd day) from their high-fiber (cereal grain and supplemental) diet to a low-fiber diet for 2 weeks and saw 41 patients move from 1 every 3.75 days to 1 every day and 16 patients from 1 every 4.19 days to 1 every 1.9 days. The 6 that stayed on the high-fiber diet saw no improvements, with some producing a mere 1 per week!
Stool frequency becomes more of valid consideration when you’re on opposite ends of the normal spectrum. For instance, excessive frequency (3+ bowel movements per day) is usually a sign of an irritable bowel, while insufficient frequency (<1 bowel movement per day) is usually tied to excessive stress – which seems to be far more common.
In 2010, hospital costs to treat constipation alone accounted for $4.25 billion – affecting nearly 30% of the population (that admits it).
If you’re not having enough bowel movements, or it’s tough to pass and looks nothing like The Perfect Poop, here are some ways to Increase Frequency (assuming you’re already following Live It NOT Diet!):
- Evaluate your stress level – more down time?
- Monitor your water intake
- Troubleshoot your diet:
- Use more oils (coconut, olive)? Fat lubes the machine.
- Prioritize fibrous vegetables (and fruit when appropriate)? The good fiber that feeds the gut.
- Eat more fish or commit to taking fish oil? Reduces inflammation.
- Add some fermented foods (or take a probiotic)?
- Cool it on the aged cheeses?
- Eat a little more salt (low carb = salt & water loss)?
- Supplement magnesium – relaxes muscles, draws water to colon
- Make time to poop – find a way to relax when it’s time to shine
- Get a Squatty Potty – ideal recto-angle
- Sit less and walk more – promotes peristalsis
Most people are quickly fixed up when they start paying attention to their water intake, get a handle on their stress, and pop a few chelated magnesium caps before bed. However, there’s also people that try all the above and still struggle.
Experience (and research) has taught me that this could be a hypoactive thyroid. Which can be reinvigorated with a few drops of iodine per day if it’s related to a deficiency, but could also be a sign of an auto-immune condition – like Hashimoto’s thyroiditis or Graves disease. So, it can be worth exploring IF your diet is on-point (and has been on-point for a while), your stress is in-check, and your GI tract is more lubed-up than Barbara the Bodybuilder.
In MOST cases it’s more sleep, more activity, more water, and more magnesium. And even if it’s low thyroid function, many times stress is the underlying cause.

Seeing undigested food in your stool has also become common in the 21st century, since a good chunk of the population has developed an underactive stomach (via antacids) and inadequate gut bacteria (via antibiotics). Along with losing the medication, you’ll want to consider an HCL supplement, and start adopting practices to improve your digestion (like eating slow, avoiding water with meals, and befriending vinegar).
Softer stools (anywhere above Type 4) are usually less common, but generally indicate some sort of reactivity. Whether that’s trouble processing a specific sugar (like lactose), a specific protein (like gluten), or an artificial sweetener. Sometimes it can mean too much of a specific food as well, with excess fruit being a common example.
If you’re already following Live It NOT Diet!, and you’re having too many bowel movements per day (or they look like Types 5-7 often), I would highly encourage you to remove all wheat from your diet (yes, even on feast days) – as this is usually a sign of gut permeability or some form of food sensitivity (gluten). And if not looked after immediately, it could result in something more serious (leaky gut, IBD, etc).
Stay Lean!
Coach Mike
RELATED ARTICLES:
How Stress Makes You Fat & Sick
